Leading the Next Chapter: Meet Apogee’s New Owner, Andrew “Andy” Richards
April 16, 2026

The coordination meeting had already run long.
On the screen was a 3D model of the surgical suite renovation. The structural grid worked…on paper. But above the ceiling, reality was setting in; a transfer beam cut through primary ductwork, medical gas mains were competing with the seismic bracing, the electrical team needed more space for redundant feeders serving the OR panel, and the architect was concerned with the ceiling height. Every discipline has a valid requirement. The plenum did not.
Just five years ago, the solution would have been familiar; adjust one system, re-run calculations, issue revised backgrounds, reconvene next week. Incremental problem-solving, one conflict at a time.
Today, the same moment can look much different.
Instead of reacting to clashes after they appear, teams can analyze coordination risk earlier. Instead of testing one framing option, they can evaluate dozens before design development hardens. Artificial intelligence (AI) is not eliminating engineering judgment in healthcare projects, but it is changing when and how that judgement is applied.
One of the most immediate applications is early stage spatial and structural optimization. Healthcare facilities are uniquely demanding. Structural systems must account for vibration-sensitive imaging equipment, concentrated surgical loads, and future flexibility. Mechanical systems must satisfy strict air change rates and pressurization relationships. Electrical infrastructure must provide redundancy without sacrificing space. At the same time, architectural planning also drives performance; clinical adjacencies influence patient outcomes, travel distances affect staff fatigue, and room proportions shape the patient experience.
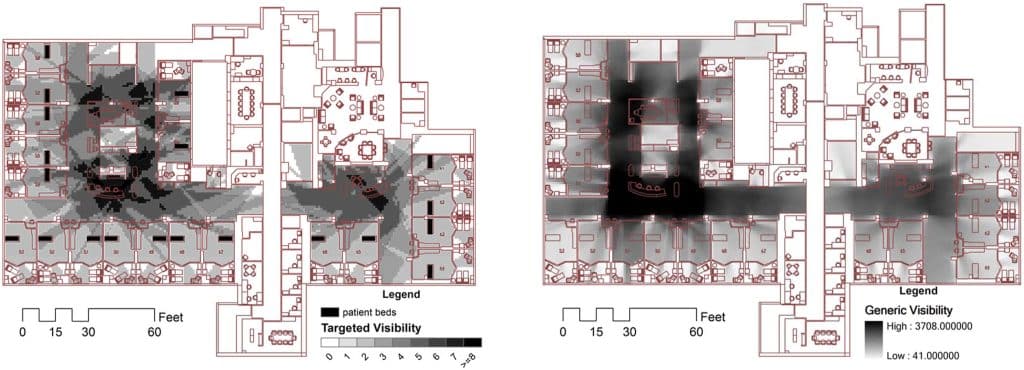
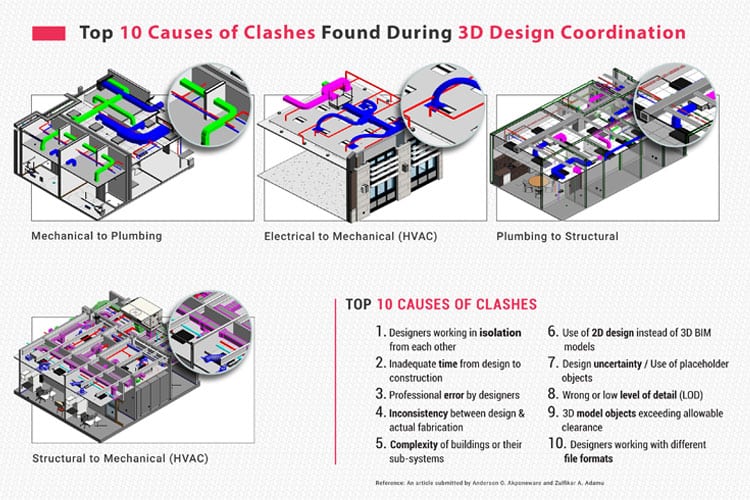
AI is also transforming architectural, MEP and structural coordination in dense clinical environments. Hospital ceilings are among the most congested spaces in any building type. Medical gas, chilled water, steam, fire protection, cable trays, lighting systems, and architectural ceiling assemblies must coexist within tight tolerances.
Machine learning enabled coordination tools can analyze clash histories across similar projects to identify recurring high-risk intersections. Instead of simply flagging conflicts after modeling, AI can predict zones where structural bracing is statistically likely to interfere with a duct or where equipment access clearances may be compromised. This shifts coordination from reactive detection to proactive mitigation.
Another critical area is code and compliance navigation. Healthcare projects must reconcile building codes, life safety provisions, energy standards, and special healthcare regulations. AI-assisted tools can rapidly parse regulatory text and highlight requirements tied to smoke compartments, egress capacity, equipment anchorage, or system redundancy.
This does not replace professional judgement or expertise. It strengthens it by reducing the risk that critical provisions are discovered late during plan review or inspections.
AI also supports resilience and operational continuity planning. Hospitals cannot afford downtime. Emergency power distribution, structural performance under seismic events, and HVAC redundancy must function under extreme scenarios. AI-enabled simulations allow engineers to compare system configurations across multiple stress conditions, evaluating performance tradeoffs more quickly and comprehensively.

Perhaps most importantly, AI enhances institutional memory. Healthcare systems often build repeatedly: renovations, expansions, satellite clinics, etc. AI tools can analyze historical RFIs, change orders, and coordination issues to detect patterns. If certain equipment loads repeatedly require late structural reinforcement, or if a specific wall finish selection generates maintenance concerns, that insight can inform earlier programming criteria on future projects.
Healthcare design is fundamentally about managing risk while improving the human experience—protecting patients, caregivers, and critical operations without losing sight of dignity and comfort. Artificial Intelligence does not assume that responsibility, licensed professionals still do. What AI offers is expanded visibility: more options explored, more conflicts anticipated, and more lessons retained.
In healthcare design, AI is not replacing the design team in coordination meetings. It is positioning the team with better information before the meeting even begins.